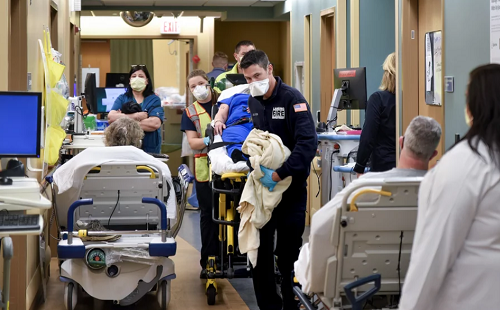
October 27, 2021 – Even in parts of the country that aren’t overwhelmed with COVID-19, patients are still filling up ERs – many of them sicker than before the pandemic, with their diseases more advanced and in need of more complex care.
Doctors and nurses say the severity of illness ranges widely and includes abdominal pain, respiratory problems, blood clots, heart conditions and suicide attempts, among others.
In the spring of 2020 when the coronavirus pandemic began, ERs across the U.S. were empty as hospitals cancelled procedures and patients who were sick with other things did their best to stay away from hospitals. But those months of treatment delays have exacerbated chronic conditions and worsened symptoms. Many patients are now reaching the point where delaying care is no longer an option, even though hospitals are stull struggling under the pressures of COVID-19.
Across the nation, emergency departments visits to dropped to half their normal levels at the start of the pandemic, and didn’t fully rebound until the summer of 2021, according to the Epic Health Research Network. Now, although the number of ER patients is mostly back to “normal,” patients are much sicker, NPR reports. This is making admission rates, from the ER to the hospital’s inpatient floors, almost 20% higher, according to the Epic Health Research Network.
“We are hearing from members in every part of the country,” says Dr. Lisa Moreno, president of the American Academy of Emergency Medicine (AAEM). “The Midwest, the South, the Northeast, the West … they are seeing this exact same phenomenon.”
In hospitals across the country, long-term care floors are full, with a mix of COVID-19 and non-COVID-19 patients. In hotspot areas, some ER patients are having to be warehoused for hours, even days, and ER staff are being called to perform long-term care roles they weren’t trained to do.
Less acute cases, such as rashes or conjunctivitis, still aren’t going to the ER as much as they used to. Instead, they may be opting for an urgent care center or their primary care doctor. Meanwhile, there has been an increase in people coming to the ER with more serious conditions, like strokes and heart attacks, NPR says.
While all categories of elective surgeries in a study from Epic Health Research Network were within 14% of predicted levels after lockdown lifted in June 2020, none appear to have fully made up the deficit of missed surgeries from early in the pandemic. Knee prosthesis and thyroid or parathyroid surgeries showed the lowest volumes compared to expected in the post-lockdown period, in addition to some of the largest drops in volume during the lockdown period.
In Wisconsin, this wave of procrastinated care is leading not only to fuller emergency departments, but many urgent care clinics and hospitals are at or above capacity and patients are having to wait longer to visit a primary care provider, according to Dr. Sandra Kamnetz, vice chair of clinical care, family medicine at UW Health and professor of family medicine and community health at the UW School of Medicine and Public Health.
WisPolitics.com reported that, in Wisconsin since July 1, 2020, preventative healthcare appointments were the most likely to be canceled, according to results from a survey conducted by the Survey of the Health of Wisconsin at the UW School of Medicine and Public Health.
Additionally, a greater number of people are reporting depression and anxiety. In June 2020, about 40% of adults surveyed in the United States reported struggling with mental health or substance abuse, according to a Centers for Disease Control and Prevention report.
The percentage of anxiety disorders reported was three times greater than the second quarter of 2019, while the prevalence of depression reported was four times greater during that time, the report showed.
