
May 10, 2021 – While the COVID-19 pandemic devastates India, much of the rest of the world is beginning to see some relief. The United States is returning to conditions unseen for months, if not since the earliest days of the outbreak.
India reported 2.6 million new cases in the last seven days, nearly half of all new cases globally. The country reported 27,000 COVID-19 deaths in the past week.
The stories of pain, fear, and suffering in this country are devastating. Most observers believe the problem is worse than even these exceptional case and death totals. The Institute for Health Metrics and Evaluation (IHME) estimates eight million people are infected in India every day. IHME estimates that new daily infections began to recede two weeks ago, offering a small measure of hope.
Outside of the United States, newly reported cases finally started dropping eight days ago. These cases had increased continuously for the preceding two months. During that time, new daily cases surged 250%.
The situation is brighter in the United States. New weekly cases fell on Saturday to the lowest point since September 21-27, 2020. That is a thirty-three-week low for this key measure. Even more encouraging, new cases are declining faster day by day.
Yet, that’s not the whole story.
Actual infections exceed detected cases by a factor of three to four times, according to the CDC. The Schools of Public Health at Harvard, Stanford, and Yale Universities collaborate on a model that estimates actual infections (covidestim.org).
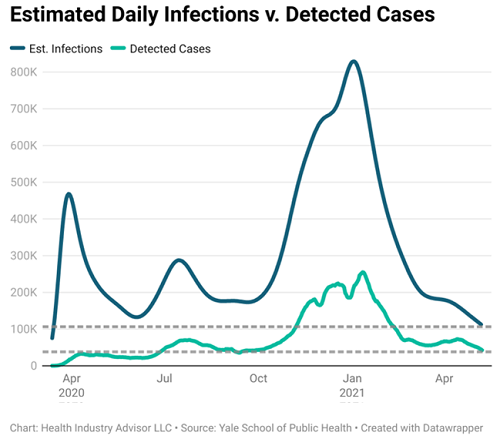
On Saturday, estimated daily infections dropped to the lowest point in the United States since March 14, 2020. Estimated daily infections have been declining continuously since January 2, plunging 86% during these 18 weeks.
Declining new cases are easing the strain on our nation’s hospitals. During at least two stretches, the pandemic had created an existential crisis in the industry. The first was in the early pandemic days. Exponential growth in novel coronavirus cases exhausted staff, beds, ventilators, and personal protective equipment. For weeks, COVID-19 patients outnumbered inpatient beds in Connecticut, New Jersey, and New York.
The second occurred toward the end of 2020. With new daily cases climbing to record levels, hospital beds in Arizona, California (especially southern California), and Utah were full of COVID-19 patients.
At its peak in early January, COVID-19 patients occupied 43% of all inpatient beds in the country.
Then the vaccination effort began to pay dividends. Targeting senior citizens first, the vaccine effort lowered the COVID-19 hospital census since the beginning of the year. As of Friday, the COVID-19 census had fallen below 12% of the nation’s inpatient beds. Even the states with the highest rates, Maryland and Michigan, see rates less than one-third of those suffered by Arizona, California, Connecticut, New Jersey, New York, and Utah on the worst days. Even better, occupancy rates are falling across the country each day.
The COVID-19 hospital census is at a six-month low.
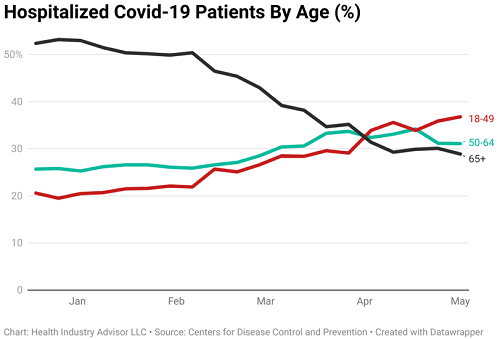
The age mix of hospital patients has shifted, however, tied to the focus of the vaccine effort. When vaccinations started, senior citizens were 2.6 times more likely to be hospitalized with COVID-19 than younger adults (18-49 years old). Seniors were seven times more likely to be hospitalized than middle-aged adults. As a result, more than half of the patients hospitalized with COVID-19 were senior citizens.
Health officials made it a priority to vaccinate these at-risk seniors first. The effort paid dividends. In the most recent data from the CDC, seniors represented a smaller percentage (29%) of hospitalized patients than both the younger (37%) and middle-aged adults (31%). Moreover, seniors were 2.4 times more likely than middle-aged adults to be hospitalized (down from seven times more likely).
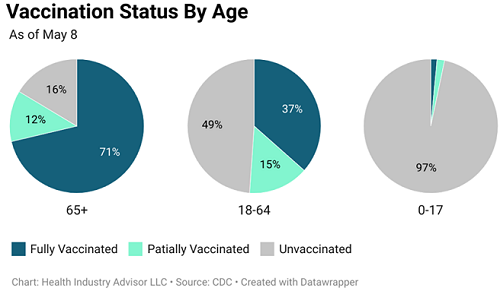
Of course, the vaccination effort has gradually involved other age groups. First, middle-aged adults joined the effort. More recently, the invitation was extended to everyone 16 years and older. (As early as this week, vaccines will include persons as young as 12 years old.)
This gradual expansion of vaccinations has played out in hospitalization rates. Middle-aged adults began to represent a declining share of hospital patients in recent weeks.
Younger adults, who have only recently been allowed to receive vaccines, now represent the highest share of COVID-19 hospital patients of any age group. Alarmingly, the likelihood of a younger adult hospitalized with COVID-19 has not improved much since the U.S. vaccination effort started. The possibility for seniors has been cut by three-fourths; the potential for middle-aged adults is half its earlier level.
Vaccinations, and the decline of severe cases, are reducing deaths with coronavirus too. In much of January, 3,300 Americans were lost each day to the virus. This rate has plunged to fewer than 700 daily throughout May. This rate is the lowest we have seen in ten months.
With these encouraging trends in cases, hospitalizations, and deaths, how soon will we return to early pandemic levels? IHME publishes a forecast each week. In its most recent estimates (May 6), IHME showed that cases as of this Saturday would fall lower than any day since March 10, 2020. Cases should continue falling well into the summer.
By May 27, COVID-19 hospital census drops to its lowest level since March 24, 2020.
Most encouragingly, IHME forecasts that as early as this Thursday, daily deaths could reach the lowest point since March 24, 2020.
With the observance of National Nurses Week, we must salute their role in making our progress possible. We could not be here today without the service and compassion of these professionals. For their sake, I sincerely hope that we continue to bring this virus under control – here and across the globe.
Contributing writer:
Mark A. Van Sumeren, strategic advisor, Medical Devices & Integrated Delivery Networks
Health Industry Advisor LLC, provides a regular report on COVID-19 numbers for the health care industry.
For more information, or to sign up for the report, contact Mark at Mark.VanSumeren@HealthIndustryAdvisor.com; or visit www.HealthIndustryAdvisor.com.
